Vulvar dermatitis, a discomforting skin condition characterized by irritation, redness, and itchiness around the vulva, often emerges as a complication of incontinence. This condition, affecting a significant number of individuals with urinary incontinence, can severely impact quality of life, emphasizing the need for effective management strategies. This blog delves into the prevalence, causes, symptoms, and treatments of vulvar dermatitis related to incontinence, offering insights backed by research and statistics to guide those affected toward relief and comfort.
The Prevalence of Vulvar Dermatitis in Incontinence
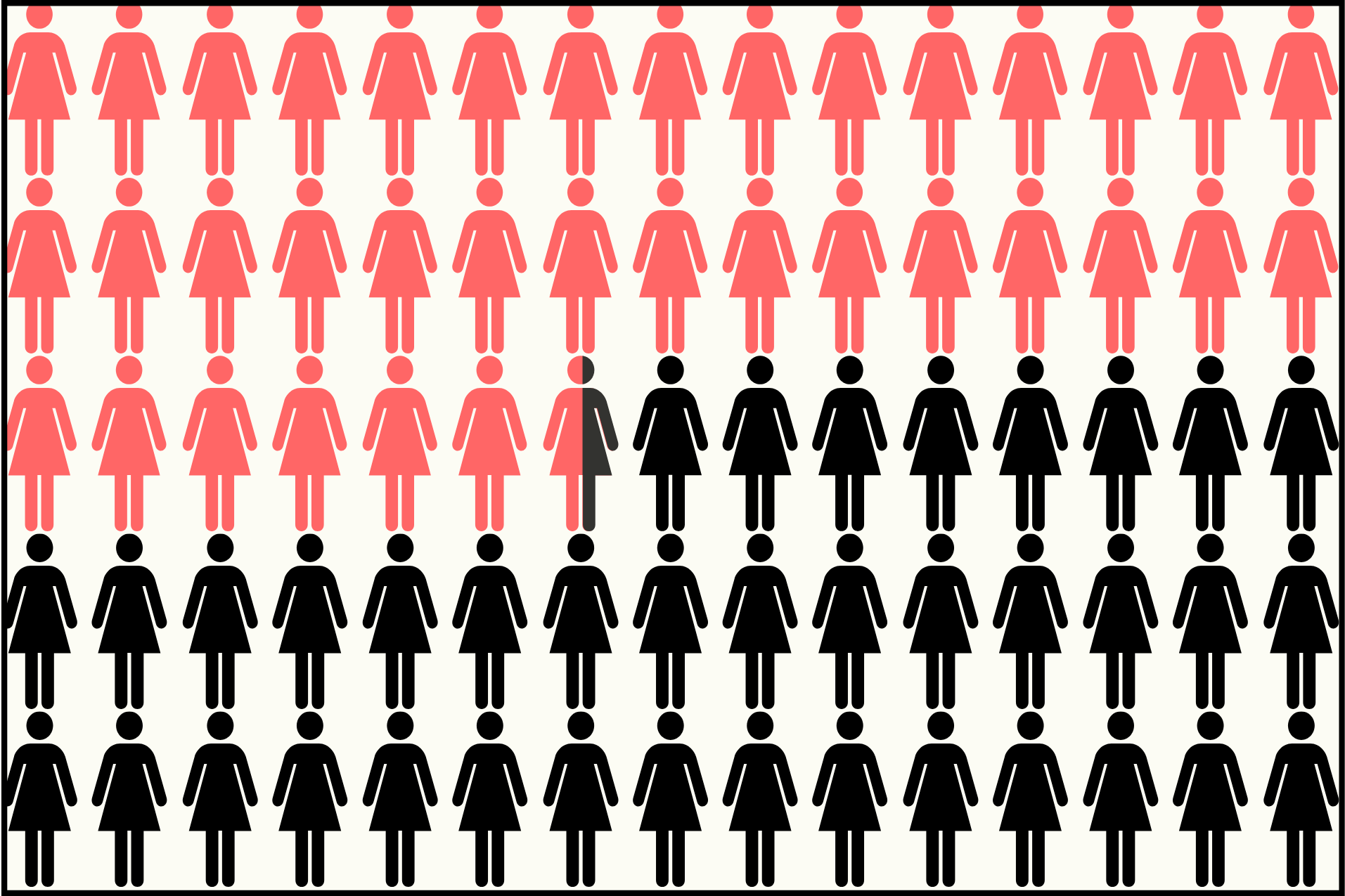
Research indicates that skin problems, including vulvar dermatitis, are common among individuals suffering from incontinence. It’s estimated that 50% of people with incontinence experience some form of skin irritation. Incontinence-associated dermatitis (IAD), including vulvar dermatitis, is not just uncomfortable but can also lead to secondary infections if left untreated.
Causes and Risk Factors
Vulvar dermatitis in the context of incontinence primarily arises from prolonged exposure to moisture and irritants found in urine and feces. This exposure disrupts the skin's natural barrier, leading to irritation, inflammation, and the development of dermatitis. Factors that increase the risk include poor hygiene, frequent urinary tract infections, and the use of incontinence pads or diapers that trap moisture against the skin.
Symptoms to Look Out For
Individuals experiencing vulvar dermatitis often report symptoms such as persistent itching, burning sensations, redness, and swelling in the vulvar area. The skin may appear cracked or scaly and, in severe cases, might develop sores or blisters. These symptoms not only cause physical discomfort but also contribute to emotional distress and social withdrawal.
Causes of Incontinence
Incontinence in women can stem from a variety of causes, often linked to underlying conditions that affect the bladder, pelvic floor muscles, or the nerves controlling them. One of the primary factors is childbirth, which can weaken the pelvic floor muscles and damage nerves, leading to stress incontinence — the leakage of urine when pressure is exerted on the bladder by coughing, sneezing, laughing, or exercising. Hormonal changes during menopause can also contribute to incontinence; the decrease in estrogen can weaken the urethra's support system, resulting in urge incontinence or an overactive bladder.
Other contributing factors include obesity, which puts additional pressure on the bladder and pelvic muscles, chronic urinary tract infections (UTIs) that may irritate the bladder, and surgeries related to the reproductive system that can affect the pelvic floor muscles. Neurological disorders, such as multiple sclerosis or Parkinson's disease, can interfere with nerve signals involved in bladder control, leading to episodes of incontinence. Understanding these causes is crucial for diagnosing and effectively treating incontinence in women, highlighting the importance of seeking medical advice for persistent symptoms.
Types of Incontinence:
- Stress Incontinence: This is the most common form of incontinence, especially among women. It occurs when physical movements or activities like coughing, sneezing, laughing, or exercising put pressure on the bladder, leading to the involuntary leakage of urine. It's often related to weakened pelvic floor muscles due to childbirth or surgery.
- Urge Incontinence: Also known as overactive bladder, urge incontinence is characterized by a sudden, intense urge to urinate followed by involuntary leakage. It can be caused by urinary tract infections, neurological disorders, or diabetes, and it's marked by frequent urination during the day and night.
- Overflow Incontinence: This type occurs when the bladder doesn't empty completely, leading to dribbling or constant leaking of urine. It's often related to bladder damage, nerve damage, or blockages in the urinary tract, and it's more common in men with prostate gland problems.
- Functional Incontinence: Functional incontinence arises not from issues with the bladder itself but from physical or mental impairments that prevent timely access to a toilet. Conditions such as severe arthritis or dementia can lead to this type of incontinence.
- Mixed Incontinence: This is a combination of stress and urge incontinence, where an individual experiences symptoms of both conditions. It's particularly common in women and can complicate diagnosis and treatment, requiring a multifaceted approach to manage the different symptoms.
- Transient Incontinence: Transient incontinence is temporary and usually caused by an underlying condition or factor that, when treated, resolves the incontinence. Common causes include urinary tract infections, acute illness, or the effects of medications.
- Bowel Incontinence (fecal incontinence): is the inability to control bowel movements, causing unintentional loss of feces from the rectum caused by an underlying problem or factor that, when treated, resolves the incontinence. Common factors include nerve damage, chronic conditions like diabetes, and chronic constipation.

Effective Treatment and Management Strategies
Barrier Creams and Protective Ointments
Barrier creams and protective ointments play a crucial role in preventing vulvar dermatitis, especially in individuals dealing with incontinence. These products work by creating a protective layer on the skin's surface, shielding it from the irritating effects of urine and feces. Ingredients like zinc oxide and dimethicone are common in these formulations, offering both moisture-resistant and soothing properties.
This protective barrier not only prevents direct contact with irritants but also helps to maintain the skin's natural moisture balance, reducing the risk of dryness and cracking. By minimizing exposure to irritants, these creams and ointments can significantly reduce the incidence of inflammation and irritation associated with vulvar dermatitis. Regular application, particularly after cleansing and before using any incontinence pads or garments, is essential for effective protection and maintenance of skin health in vulnerable areas.
Gentle Skin Care
Gentle skincare is pivotal in preventing vulvar dermatitis, particularly for those susceptible due to incontinence. This approach involves using mild, non-irritating cleansers that are free from harsh chemicals, fragrances, and dyes, which can exacerbate skin sensitivity and irritation. After cleansing, it's crucial to pat the area dry gently with a soft towel or wipe rather than rubbing, to avoid further irritation or damage to the skin.
Additionally, applying moisturizers that are specifically formulated for sensitive skin can help maintain the skin's natural barrier function, keeping it hydrated and less prone to cracking or peeling. Avoiding products with alcohol, fragrances, and other potential irritants is essential in minimizing the risk of flare-ups.
By adopting a regimen centered on gentle skincare, individuals can significantly reduce the likelihood of developing vulvar dermatitis, maintaining healthy and resilient skin even in the face of challenges like incontinence.
Frequent Changes
Frequent changes of incontinence products are essential in preventing vulvar dermatitis, a condition exacerbated by prolonged exposure to moisture and irritants found in urine and feces. Staying in wet or soiled incontinence pads, diapers, or underwear creates a humid environment that not only irritates the skin but also promotes the growth of bacteria and fungi, increasing the risk of infection and skin breakdown. Regularly changing these products helps to keep the skin dry and reduces exposure to irritants, significantly lowering the chance of developing dermatitis.
Additionally, opting for incontinence products with breathable materials can further enhance skin health by allowing air circulation, which helps to evaporate trapped moisture and keep the skin cool. This practice, combined with proper skin care routines, forms a comprehensive approach to managing incontinence while minimizing the risk of skin complications like vulvar dermatitis.
Types of Incontinence Products:
- Incontinence Underwear or Diapers: Adult diapers are specialized garments designed to manage and contain urinary or fecal leakage. Unlike standard underwear, incontinence underwear is made with absorbent materials capable of holding varying amounts of liquid, effectively preventing leaks and odors. These products are available in a range of sizes and absorbency levels to accommodate different degrees of incontinence, from light to heavy flow.
- Incontinence Pads or Guards: Incontinence pads are specially designed absorbent pads made to manage symptoms of urinary incontinence. Unlike regular sanitary napkins, incontinence pads are specifically engineered to handle the rapid flow of urine, featuring super-absorbent materials that lock moisture away from the skin, thus reducing the risk of irritation and discomfort. Incontinence guards are similar, but are specifically designed to file the male anatomy. Available in a variety of shapes, sizes, and absorbency levels, incontinence pads cater to a wide range of needs, from light spotting to heavier flows associated with urge incontinence.
- Booster Pads: Incontinence boosters, also known as booster pads or inserts, are designed to enhance the absorbency of primary incontinence products like briefs, pull-ups, or underpads. These slim, absorbent layers are intended to be placed inside the primary incontinence garment to provide additional protection against leakage, especially for individuals with moderate to heavy incontinence. Unlike standard incontinence pads, boosters do not have a waterproof backing. This design allows liquid to pass through the booster pad once it reaches its maximum absorbency, then into the primary absorbent garment beneath, maximizing the overall capacity of the incontinence protection and extending the wear time of the primary garment.
Medical Treatment
Medical treatments for vulvar dermatitis are designed to alleviate symptoms and address the underlying causes of irritation.
Corticosteroids:
Depending on the severity and the presence of secondary infections, healthcare providers may prescribe topical corticosteroids to reduce inflammation and itching. These steroids vary in strength and are applied directly to the affected area, offering relief from the discomfort associated with dermatitis.
In cases where a yeast or bacterial infection is identified as a contributing factor to the skin irritation, antifungal or antibiotic medications may also be prescribed to eliminate the infection and prevent further exacerbation of dermatitis symptoms.
It's crucial for patients to follow their healthcare provider's instructions closely when using these medications, as improper use can lead to skin thinning or other side effects. Through a combination of targeted medical treatments and supportive care, individuals can achieve significant relief from vulvar dermatitis, improving their quality of life.
Topical Estrogen:
Topical estrogen is prescribed for vulvar dermatitis primarily in cases where the condition is linked to estrogen deficiency, such as in postmenopausal women or those who have undergone certain medical treatments that affect estrogen levels. This hormonal deficiency can lead to vulvar atrophy, where the skin and mucosa of the vulva become thinner, drier, and more susceptible to irritation and inflammation. When symptoms of vulvar dermatitis are believed to be exacerbated by these changes, healthcare providers may recommend topical estrogen therapy.
This treatment involves the application of estrogen directly to the affected area, which helps to restore the natural thickness, elasticity, and moisture of the vulvar skin, thereby alleviating the symptoms of dermatitis. Topical estrogen is typically considered after other causes of dermatitis have been ruled out or managed, and it is used cautiously, taking into account the patient's overall health, history of hormone-sensitive conditions, and the potential risks and benefits of hormone therapy.
Lifestyle Modifications:
Lifestyle modifications play a crucial role in preventing vulvar dermatitis, particularly for individuals prone to this condition due to factors like incontinence. One key strategy is maintaining optimal hygiene while being mindful not to over wash or use harsh, irritating products on the sensitive vulva area. Using unscented, hypoallergenic soaps and avoiding douches, scented wipes, and bubble baths can help maintain the natural pH balance and prevent irritation. Wearing loose, breathable clothing, and opting for cotton underwear can also reduce moisture buildup, which is a common irritant. For those with incontinence, changing protective pads or underwear frequently to avoid prolonged exposure to moisture is essential.
Additionally, managing dietary factors that may exacerbate incontinence, such as limiting intake of caffeine and alcohol, can indirectly help prevent vulvar dermatitis by reducing bladder irritants. Incorporating these lifestyle changes can significantly lower the risk of developing vulvar dermatitis, promoting healthier skin and reducing discomfort.
Vulvar dermatitis caused by incontinence poses a significant challenge to those affected, impacting not only their physical health but also their emotional wellbeing. Understanding the causes and symptoms is the first step toward effective management. With proper care, the right products, and medical guidance, individuals can find relief from the discomfort of vulvar dermatitis. It's essential for those experiencing symptoms to consult healthcare professionals to develop a tailored treatment plan that addresses both incontinence and its dermatological complications.
If you're struggling with incontinence, join one of our private support groups today!
Women's Incontinence Support Group
Men's Incontinence Support Group
Sources:
Cleveland Clinic. (n.d.). Vulvar Dermatitis. Cleveland Clinic. Retrieved from https://my.clevelandclinic.org/health/diseases/24336-vulvar-dermatitis
Holroyd, S. (2024). Moisture-associated skin damage caused by incontinence. Journal of Community Nursing, 35(4): 58-64. https://www.ucc-today.com/journals/issue/launch-edition/article/moisture-associated-skin-damage-incontinence
Mac Bride, M. B., Rhodes, D. J., & Shuster, L. T. (2010). Vulvovaginal atrophy. Mayo Clinic proceedings, 85(1), 87–94. https://doi.org/10.4065/mcp.2009.0413











